A Review and Update on the Biochemical Basis of Conscious Breathing (Pranayama)
Abstract
Breathing has long been recognised as a vital process in Eastern traditions such as YOGA and Ayurvedic medicine, where Pranayama is regarded as a transformative practice that harmonises body and mind. While the East developed sophisticated systems of breath regulation for health and self-awareness, the West largely overlooked their significance until the late 19th and early 20th centuries. A group of pioneering physicians, sometimes referred to as "the pulmonauts", including Christian Bohr, Konstantin Buteyko, and Peter M Litchfield, explored the physiological foundations of respiration. They emphasised the benefits of slow, nasal breathing and its relationship to both physical and emotional well- being. In the 21st century, contemporary researchers and practitioners such as James Nestor, J. Patrick McKeown and Anders Olsson have expanded this understanding through the fields of biochemistry, physiology, and biomechanics.
Their work has clarified the mechanisms underlying conscious breathing and refined ancient pranayama techniques. Integrating insights from both Eastern and Western traditions reveals that breathing is a central factor in maintaining homeostasis and emotional balance.
Author Contributions
Academic Editor: Anubha Bajaj, Consultant Histopathologist, A.B. Diagnostics, Delhi, India
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2026 Carlos Aulesa, et al.
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
Each author declares that they have no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangement, etc.) that might pose a conflict of interest in connection with the submitted article.
Citation:
Introduction
The importance of breathing has long been recognised in Eastern traditions such as YOGA and Ayurveda, a millennial Medicine. The term pranayama comes from Sanskrit, where prana means “vital energy” and ayamatranslates as “control” or “expansion.” Pranayama is more than just a simple breathing technique; it is a transformative practice that regulates vital energy through conscious breath control 1.
Despite its essential role in health and well-being, breathing has often been overlooked in the West. Between 1870 and 1950, however, a group of physicians known as “the pulmonauts”, including Christian Bohr(1904)[2], Konstantin Buteyko(1923) [3], studied and promoted healthy breathing habits. They emphasised slow, relaxed, nasal breathing during rest. Research has shown a strong connection between dysfunctional breathing patterns and physical and emotional health. Stressful breathing, for example, can lead to hypoxia (insufficient Oxygen), which in turn affects the brain and generates feelings of anxiety, fear, and distress.
The work of these Western physicians, together with the wisdom of Eastern traditions like Yoga and Ayurveda, and modern practices such as mindfulness and meditation, all highlight the central role of breathing in maintaining the balance of body, mind, and emotions 4. Conversely, in the 21st century, modern Western followers of the Pulmonaut school, such as Olson A. 5, Nestor J. 6, and McKeown P. 7, 8, have applied their knowledge of blood chemistry, physiology, anatomy, and the biomechanical mechanisms that underlie conscious breathing. At the same time, they have contributed to a deeper understanding and refinement of pranayama practice.
The purpose of this work is to compile, explain, and actualise these pranayama techniques from a biochemical, physiological and anatomical perspective to facilitate their comprehension and application in alternative medicine.
Materials And Methods
Pranayama (The Science of Conscious Breathing)
Pranayama is a core practice in Yoga that focuses on controlling and expanding vital energy (prana) through the breath. Mentioned in Patanjali’s Yoga Sutras, it is regarded as the fourth limb of Yoga and is designed to prepare both body and mind for deep meditation. The basic practice includes techniques such as abdominal breathing (Adhama Pranayama), complete or yogic breathing (Dirgha Pranayama), and alternate nostril breathing (basic Nadi Shodhana), and advanced techniques such as Anulom Vilom, Bhastrika, and others, each producing specific effects on balance, energy, and mental calm1. Their benefits include improved lung capacity, regulation of the nervous system, stress reduction, and enhanced concentration and mental clarity 4. It's recommended to practice in a quiet setting, maintaining good posture and focusing on your breathing. When integrated with asanas and meditation, Pranayama enhances overall well-being and fosters greater physical and mental9, 10
Physiology of Breathing
The cells and organs of our body constantly consume Oxygen and produce large amounts of carbon dioxide. Breathing is one of our most fundamental functions, as it provides the body with Oxygen while removing carbon dioxide 11. Oxygen enters the lungs through the nasal passages and throat, then passes down the trachea, which branches into increasingly smaller tubes within the lungs, ending in tiny sacs called alveoli. Each alveolus is surrounded by minute blood vessels known as capillaries, which allow Oxygen to pass into the bloodstream while collecting waste products. The alveoli are clustered like bunches of grapes, and each lung contains several hundred million of them. Once the air reaches the lungs, it fills the alveoli, and Oxygen diffuses into the blood, which is carried by haemoglobin in red blood cells to every cell in the body. At the same time, the blood releases carbon dioxide into the alveoli, which is then exhaled. This waste, transported by haemoglobin, leaves the body as the alveoli deflate and empty of the gases they have collected 12, 13. During breath holding, following normal breath patterns (inhalation, exhalation, break hold-time), oxygen levels drop, and carbon dioxide levels increase. This causes acidosis in humans by increasing blood CO₂, decreasing blood pH, and reducing oxygen affinity, which facilitates oxygen delivery to tissues. Most importantly, CO₂ determines the bioavailability of Oxygen to the tissues and cells; it is not always a waste gas.
Nose and paranasal sinuses
An essential element in Pranayama is breathing through the nose. From an anatomical point of view, the nose is composed of the external nasal pyramid, the nasal cavities, the nasal septum, the turbinates (superior, middle, and inferior), and the paranasal sinuses (frontal, ethmoidal, sphenoidal, and maxillary)14, 15. The nasal cycle depends on erectile tissue that acts as an air-conditioning system for inspired air, regulating its temperature, humidity, and airflow resistance. In addition, the nasal mucosa produces chemical substances such as nitric oxide (NO), a powerful vasodilator that contributes to normal respiratory function. Breathing through the nose results in a 10-20% increase in oxygen uptake in the blood. During breathing, the nasal cilia move the mucus backward and downward, functioning like a conveyor belt that cleans and filters the inspired air, and represents an important first line of defence against infection. Furthermore, breathing through the mouth leads to greater water loss. Studies show that up to 42% more water is lost during mouth breathing compared to nasal breathing. In contrast, breathing through the nose helps retain moisture and therefore plays an important role in preventing dehydration8.
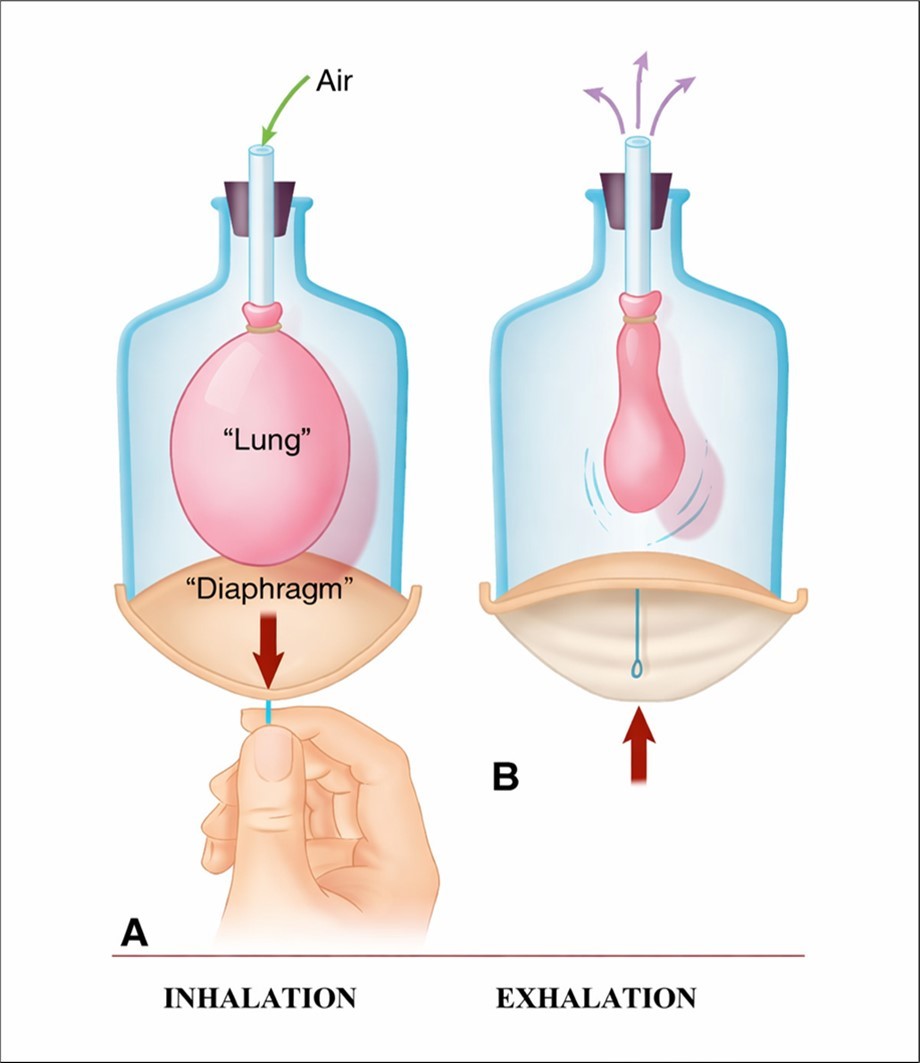
Neuromuscular Mechanisms of Respiration: The Diaphragm and the Phrenic Nerve
The diaphragm, often called “the second heart,” is the primary muscle responsible for breathing. During inhalation, the diaphragm contracts and moves downward, expanding the lungs and allowing air to enter. During exhalation, the diaphragm relaxes and rises, reducing lung volume and aiding air expulsion (Figure 1). The phrenic nerve innervates the diaphragm. It originates in the cervical spinal cord and travels downward to reach the diaphragm, a thin muscle located below the lungs and heart that separates the thoracic and abdominal cavities. Its primary function is to regulate the contraction and relaxation of the diaphragm, thereby controlling the breathing process 14. Forcing exhalation can make the following inhalation deeper and more effective. Under quiet breathing conditions, the diaphragm performs approximately 70-80% of the respiratory work. At the same time, the remaining effort comes from accessory muscles such as the scalenes, external intercostals, sternocleidomastoid, and parasternal intercostals15.
Acid-Base System: Biochemical Mechanism of Gas Exchange
The human body maintains blood pH within a very narrow range, between 7.35 and 7.45, since even small variations can disrupt essential enzymatic and metabolic processes11, 12. To maintain this acid-base balance, three primary mechanisms work in coordination: plasma buffer systems, the respiratory system, and the renal system.
Buffer systems rapidly neutralise changes in hydrogen and hydroxyl ion concentrations (HCO₃⁻); the most important is the bicarbonate buffer, which operates through a chemical reaction13.
CO₂ + H₂O ↔ H₂CO₃ ↔ H⁺ + HCO₃⁻
The respiratory system helps regulate pH by controlling the amount of carbon dioxide in the blood: when pH decreases (acidosis), breathing rate increases to eliminate CO₂ and reduce carbonic acid, whereas when pH rises (alkalosis), breathing slows down to retain CO₂ and restore balance11, 12. These alterations in blood pH can have significant physiological consequences: severe acidosis may impair enzyme function, reduce oxygen delivery to tissues, and cause symptoms such as confusion, fatigue, and shortness of breath, while severe alkalosis can lead to dizziness, tingling sensations, muscle spasms, and decreased cerebral blood flow. Even subtle shifts in blood pH automatically trigger respiratory adjustments to maintain equilibrium, processes in which the vagus nerve plays a central regulatory role13.
The renal system regulates pH by excreting hydrogen ions in the urine and adjusting the reabsorption or excretion of bicarbonate. Although it acts more slowly than the respiratory system, it produces a long-lasting effect by restoring and maintaining the body's acid-base balance over time12. The kidneys secrete erythropoietin (EPO), a hormone released in response to low oxygen levels in the blood. One of EPO’s primary functions is to stimulate the production and maturation of red blood cells in the bone marrow, which enhances oxygen delivery to the muscles 13.
In summary, oxygen transport and gas exchange rely on the reversible binding of oxygen to haemoglobin in red blood cells, forming oxyhaemoglobin in the lungs. During inhalation, oxygen reaches the alveoli and diffuses into the bloodstream along its concentration gradient. Carbon dioxide, in contrast, is transported in three main forms: dissolved in plasma (7–10%), bound to haemoglobin (20–30%), and predominantly as bicarbonate ions (60–70%) through the action of the enzyme carbonic anhydrase 11. Haemoglobin’s affinity for oxygen is not fixed but is influenced by several physiological factors that modify its molecular conformation. One of the most important is the Bohr effect, whereby a decrease in pH reduces haemoglobin’s affinity for oxygen. In acidic conditions, protons bind to haemoglobin, stabilising its tense (T) state, which facilitates oxygen release to the tissues 12. This mechanism is especially relevant in metabolically active tissues, where increased production of carbon dioxide and lactic acid lowers pH and promotes oxygen unloading precisely where demand is highest. In addition to low pH, elevated CO₂ levels, increased temperature, and the presence of 2,3-bisphosphoglycerate (2,3-BPG), a compound synthesised by erythrocytes in response to hypoxia,further reduce haemoglobin’s oxygen affinity, enhancing tissue oxygenation, particularly in exercising muscles 12, 13.
Although medical education often portrays oxygen as purely beneficial and carbon dioxide as harmful, physiological evidence shows that an adequate concentration of carbon dioxide in the blood is essential for maintaining normal health and effective oxygen delivery 8. Most importantly, carbon dioxide plays a key role in regulating the availability of Oxygen to tissues and cells. In other words, carbon dioxide should not be considered merely a waste gas. Some authors even advocate carbon dioxide–based therapies, giving rise to schools of thought aligned with these therapies5, 16, 17.
Vagus Nerve: Physiology and Biochemical Mechanisms
The vagus nerve, also known as the tenth cranial nerve (CN X), originates in the brainstem, the lowest part of the brain, and extends through multiple branches that reach the heart, respiratory system, and gastrointestinal tract, continuing down to the deepest viscera of the abdomen. Approximately 80–90% of its fibres are afferent, meaning they transmit information from the body to the brain, while the remaining efferent fibres innervate organs such as the heart. The vagus nerve, therefore, forms an essential communication link between the brain, heart, and lungs18. It regulates vital processes such as heart rate, respiration, and digestion, and numerous studies have shown its positive influence on physical, mental, and cognitive well-being19. Vagus nerve activity helps counteract excessive levels of cortisol, the stress hormone responsible for the fight-or-flight response20. The main neurotransmitter associated with the vagus nerve is acetylcholine12, 13, which plays a crucial role in regulating the body's autonomic functions. By releasing acetylcholine, the vagus nerve slows the heart rate, stimulates digestion, and balances the effects of the sympathetic system 18. The Heart Rate Variability Test (HRV), middlevagaltone, measuresthedifferencebetween consecutive heartbeats and iscontrolledbytheautonomicnervoussystem (ANS) [21]. The HRV is measured using devices that record heart activity, such as validated wearable devices (e.g., smartwatches). These devices detect the time between successive heartbeats and calculate variability using specialised software. Controlled breathing techniques, such as Pranayama, can stimulate the vagus nerve, activate the parasympathetic nervous system, reduce heart rate, and improve heart rate variability (HRV), a key indicator of stress resilience 22. These practices also help regulate blood pH by modifying ventilation and blood Flow23.
Physiological Control of Breathing and Blood Pressure: The Roles of Chemoreceptors and the Baroreflex
Breathing and blood pressure are controlled by chemoreceptors and the baroreflex24. Chemoreceptors detect changes in Oxygen and carbon dioxide levels in the blood. When CO₂ increases, breathing becomes faster and deeper; when CO₂ decreases, breathing slows. This helps keep the body in balance. Blood pressure is regulated by the baroreflex, using receptors in the aorta and carotid arteries. High blood pressure slows the heart rate and relaxes blood vessels, while low blood pressure increases heart rate and constricts blood vessels. Breathing and heart rate are closely connected 25. Their coordination improves oxygen exchange, heart rate variability, and nervous system balance. Chemoreceptors also interact with brain areas involved in emotion, such as the amygdala. Certain practices, such as controlled breathing techniques like Pranayama, may improve vagal tone and chemoreceptor balance. Interestingly, stimuli such as spicy foods, acupuncture, and breathing practices are thought to increase "prana," enhancing vagal and chemoreceptive balance24. For example, breath holding after exhalation increases CO₂ levels in the blood, enhancing oxygen release from red blood cells to body tissues. With practice, sensitivity to carbon dioxide decreases, and breath-hold capacity improves26. Historically, mixtures of 20% CO₂ and 70% O₂ were used therapeutically to treat anxiety, panic, and schizophrenia16, 17.
Advanced breathing techniques of Pranayama
Kapalabhati, or skull-shining breath, is characterised by rapid, forceful exhalations with passive inhalations, which quickly expel CO₂ and induce a temporary respiratory alkalosis; it also enhances cerebral oxygenation, stimulates the central nervous system, and may help relieve metabolic fatigue27
Anulom Vilom, or a variant of NadiShodhana, is a breathing technique derived from Nadi Shodhana and commonly referred to as alternate-nostril breathing. It consists of a controlled cycle of inhalation through one nostril, brief breath retention, and exhalation through the opposite side. This pattern encourages mild carbon dioxide retention, supports physiological pH stability, and contributes to stress reduction by balancing sympathetic and parasympathetic nervous system activity. Functional differences between nostrils have been documented: airflow through the right nostril is linked to increased sympathetic dominance, reflected in elevated heart rate, arterial pressure, and cortisol secretion, as well as greater engagement of the left prefrontal cortex, an area associated with imaginative and creative processing and heightened emotional reactivity. In contrast, the predominance of left-nostril breathing favours parasympathetic regulation, facilitating relaxation responses, lowering cardiovascular parameters, and alleviating anxiety, while preferentially activating right-hemisphere networks involved in linguistic, logical, and quantitative functions 28.
Bhastrika, also known as bellows breathing or Breath of Fire, consists of rapid and forceful inhalations and exhalations that markedly increase pulmonary ventilation. This heightened breathing pattern enhances oxygen intake but simultaneously accelerates CO₂ elimination, producing an energising effect. However, excessive or prolonged practice may lead to hypocapnia (PCO₂ < 35 mmHg) 29, which can result in respiratory alkalosis, dizziness, cerebral vasoconstriction, and transient cerebral hypoxia 30.
Kumbhaka, or breath retention is a pranayama technique that involves the conscious retention of the breath,following inhalation or exhalation, temporarily increases CO₂ levels, stimulates the Bohr effect, enhances oxygen release to tissues, and may induce a profound sense of calm. 30.
Ujjayi pranayama is a yogic breathing technique characterised by slow, deep inhalations and exhalations through the nose, with a gentle contraction of the glottis. This creates a soft, steady sound similar to ocean waves. It is used to calm the mind, enhance concentration, and regulate breathing rhythm, and is commonly practiced during asana practice and meditation 4, 10.
Bhramari Pranayama (Bee Breath) is a calming breathing technique where one inhales deeply through the nose and exhales while producing a humming sound like a bee. It helps reduce stress, anxiety, and mental tension, improves focus, and promotes relaxation and better sleep4, 10
Tibetanpranayama, commonly known as tummobreathing, is characterised by slow, controlled nasal breathing combined with breath retention and deliberate activation of the abdominal and pelvic musculature. This practice has been shown to increase body temperature through thermogenesis while preserving or elevating arterial CO₂ levels. The controlled hypoventilation inherent to tummo enhances tolerance to CO₂ and facilitates oxygen release to tissues via the Bohr effect, particularly in metabolically active regions29.
Results
Pranayama, a core practice of Yoga focused on conscious breath control, has a significant effect on human physiology, particularly on acid-base balance and homeostasis. By modifying breathing rate and depth, Pranayama regulates carbon dioxide (CO₂) levels and blood pH. Rapid breathing techniques increase CO₂ exhalation, leading to hypocapnia and a mild respiratory alkalosis. In contrast, slow promotes CO₂ retention, inducing mild respiratory acidosis and enhancing oxygen release to tissues through the Bohr effect.
Pranayama is a non-invasive technique that can be applied in various clinical situations: In arterial hypertension, which is associated with autonomic imbalance and oxidative stress, both linked to cellular pH alterations, technique such as and Nadi Shodhana or Bhramari Pranayama activate the parasympathetic system, reduce blood pressure, improve oxygenation, and stabilise pH. Severals clinical trials, reporting significant reductions in both systolic and diastolic pressure[31]. In conditions such as diabeticketoacidosis, characterised by severe metabolic acidosis resulting from the accumulation of ketone bodies, respiratory physiology plays a critical compensatory role. During the acute phase, hyperventilation is an essential mechanism that facilitates the elimination of carbon dioxide (CO₂), Bhastrika breathing and helps limit further reductions in blood pH. Through these indirect mechanisms, controlled breathing practices may support long-term metabolic homeostasis and improved glycaemic control.32, 33. In cardiovascular diseasessuch as chronic heart failure, which are associated with tissue hypoxia and metabolic acidosis due to reduced blood flow. Controlled breathing techniques, such as Ujjayi or Bhramari Pranayama enhance oxygenation and optimise gas exchange by reducing the respiratory rate, which in turn decreases cardiac workload and helps stabilise acid-base balance. 31. In obstructive sleepapnea(OSA), which is characterised by recurrent interruptions of breathing during sleep that result in hypercapnia, hypoxia, and fluctuations in blood pH. Diaphragmatic and conscious deep breathing as Ujjayi pranayama can enhance respiratory muscle control and reduce the frequency of apnea episodes by promoting more stable breathing patterns. Slow, deep breathing has also been shown to increase vagal tone, thereby improving sleep quality. In addition, slow, controlled breathing may stimulate melatonin production, an essential sleep-inducing hormone that has been shown to enhance vagal tone further and inhibit sympathetic nervous system activation 34. Asthma, COPD (Chronic obstructive pulmonarydisease) and someallergicdiseases: characterised by breathing difficulty. During symptoms, patients may breathe excessively, leading to hyperventilation and a reduction in blood carbon dioxide (CO₂) levels. This can cause vasoconstriction, reduced oxygen delivery to the brain, and increased brain excitability and anxiety. Nasal breathing and the Buteyko method, Ujjayi pranayam, or wearing MyoTape 6, will help bring the lips together to ensure nasal breathing, which aims to reduce hyperventilation, encourage nasal breathing, and promote slow, gentle, and controlled breathing. This may help improve symptom control when used alongside appropriate medication. In chronicpain and inflammatoryconditionssuch as rheumatoid arthritis, which are linked to chronic inflammation, oxidative stress, and local pH alterations, Ujjayi breathing supports mitochondrial function and cellular oxygenation, stabilises pH, and reduces oxidative stress through parasympathetic activation35. Renal insufficiency: gentle breathing practices such as slow, deep breathing, Nadi Shodhana (performed without breath retentions), and mild Bhramari pranayama may be considered as complementary interventions in clinically stable patients with chronic kidney disease. These techniques may help reduce psychological stress, support autonomic nervous system balance, and improve overall quality of life. DysfunctionalBreathingSyndrome: This syndrome encompasses a range of conditions affecting the neuromusculoskeletal system and the biomechanical function of the diaphragm, including disorders such as low back and neck pain, scoliosis, kyphosis, and pelvic floor dysfunctions, as well as neuromuscular and neurodegenerative diseases such as amyotrophic lateral sclerosis (ALS), Parkinson's disease, multiple sclerosis, and various muscular dystrophies. These alterations may compromise regulation of intra-abdominal pressure (IAP), lead to inefficient breathing patterns such as hyperventilation, and cause physiological imbalances (respiratory alkalosis, hypercapnia, and hypoxia), resulting in symptoms such as fatigue, headaches, dizziness, and dyspnea 29. Advanced breathing control techniques, such as the Buteyko method, are useful as adjuncts to physical and postural rehabilitation and, together with specific pharmacological treatment, may improve respiratory parameters.Furthermore, during intense exercise, when lactic acid accumulation can induce transient metabolic acidosis, fatigue, and decreased performance, post-exercise breathing practices such as slow, deep breathing and gentle forms of advanced techniques like Ujjayi pranayama (performed without breath retentions) can accelerate the recovery of acid-base balance, improve muscle oxygenation, and reduce metabolite accumulation13, 23. Finally, in cases ofanxiety, panic, and stress-related disorders, anxiety-induced hyperventilation can lead to respiratory alkalosis, producing symptoms such as dizziness, tingling, and shortness of breath. Clinical research has shown that breathing techniques such as Anulom Vilom and slow, deep breathing help restore acid-base balance by normalising CO₂ levels, reduce sympathetic hyperactivity, and significantly decrease both the frequency and intensity of panic attacks 17, 30.Anexercise to help stop a panic attack: BreathingintoCupped Hands. At thefirstsignof a panicattack, cup yourhandsacrossyourmouth and nose and gentlyslowdownyourbreathing(Figure 2). Ifyou can breatheslowly and lowwith lateral expansion and contractionofthelowerribs, thengreat. Otherwise, concentrateonbreathingslowly. CuppingyourhandswilltrapCO₂ fromyourexhaledbreath, allowingyoutorebreatheit back intoyourlungs. ThiswillincreaseCO₂ in theblood, whichwillimprovebloodflow and oxygendeliverytoyourbrain[30]. A moderate elevation in carbon dioxide tension facilitates oxygen release to cerebral tissues via the Bohr effect, thereby promoting physiological relaxation(30).However, the traditional practice of breathinginto a paper bag (Figure 3) presents significant clinical limitations 36. Re-inhalation of exhaled air may result in hypoxemiaand an unregulated rise in CO₂, potentially leading to syncope,cognitive impairment, and exacerbation of symptoms, particularly in individuals with underlying respiratory or cardiovascular disease. However, in non-clinical settings, the paper bag technique is still used in extreme situations despite the aforementioned clinical limitations.In addition, there are therapies based on breath retention and training with different concentrations of CO₂. For instance, exposure to 30% PCO₂ can trigger a panic attack, whereas lower concentrations (15% or even 7%) are used to train chemoreceptors without significantly affecting oxygen levels16, 17, 26.
Figure 2.Exercise to help stop a Panic Attack: breathing into cupped Hands
Figure 3.Exercise to help stop a Panic Attack: Breathing through a bag
Vagusnervestimulation (VNS) through prolonged exhalation has been shown to provide significant benefits for physical, mental, and cognitive health. It can reduce anxiety and depression, modulate immune function, inhibit inflammation, and promote both physiological balance and emotional regulation 18, 19. The test HRV, which measures the variability between consecutive heartbeats, is widely regarded as a reliable indicator of vagal tone and autonomic nervous system balance. 21, 22 Slow breathing at a rate of 4.5 to 6.5 breaths per minute has been shown to optimise sympathovagal balance, creating an ideal balance between sympathetic and parasympathetic activity 37. Researchers also propose that enhancing vagal tone may help explain the connection between breathing and emotional regulation 9. Independent vagal stimulation, through various pathways, is currently being explored as a therapeutic strategy for several neurological conditions, including autism and other neurodivergent disorders, such as through neuro-fascial release techniques 20. In 2017, Dr Singh reported that CO₂ stimulates the vagus nerve and acts as a natural sedative; insufficient CO₂ may therefore contribute to anxiety, depression, and irritability. He even describes carbon dioxide as "the breath of life" 38.
Furthermore, Pranayama, an accessible and non-invasive practice, has gained increasing attention as a therapeutic complement for clinical conditions that affect acid-base balance. It enhances oxygenation and cellular energy efficiency by improving oxygen saturation, particularly in poorly ventilated lung regions, through slow, deep breathing. Breath retention (Kumbhaka) further optimises oxygen uptake by prolonging haemoglobin-oxygen interaction. In addition, Pranayama supports acid-base homeostasis during stress by reducing sympathetic activation, oxidative stress, and stress-induced acidosis39. Under conditions such as intense exercise or ketoacidosis, it may facilitate recovery by promoting CO₂ elimination and regulating hydrogen ion production. Techniques such as Nadi Shodhana contribute to pH stability by balancing sympathetic and parasympathetic activity, thereby supporting overall physiological homeostasis. These therapeutic applications, however, must be accompanied by safety considerations: prolonged hyperventilation with techniques such as Kapalabhati or Bhastrika should be avoided to prevent dizziness or cerebral hypoxia; practices must be adapted for patients with severe renal or respiratory failure and for beginners. Should start gradually with gentle techniques such as Nadi Shodhana before progressing to more intense methods27.
Discussion
Breathing, beyond its basic physiological function, profoundly influences the neurological, cardiovascular, endocrine, and mental health systems. Because breathing is an innate bodily function which most of us take for granted, it only gets our attention when something goes wrong. Scientific evidence shows that both the breathing pattern and the dominant nostril can directly modulate the activity of the autonomic nervous system 23. Right-nostril breathing is associated with sympathetic activation, increasing heart rate, blood pressure, and cortisol levels. It also stimulates the left prefrontal hemisphere, linked to creativity and imagination, as well as to greater sensitivity to negative emotions. Conversely, left-nostril breathing activates the parasympathetic system, promoting relaxation, lowering blood pressure, and reducing anxiety, while enhancing right-hemisphere activity associated with logic, language, and analytical reasoning 28. Nasal breathing offers multiple advantages. It filters and conditions inhaled air, stimulating the production of nitric oxide (NO). This potent bronchodilator enhances oxygen absorption by up to 18% and increases PCO₂ (Partial pressure of Carbon dioxide), promoting vasodilation and optimising gas exchange 23. In addition, breathing through the nose helps retain moisture and therefore plays an important role in preventing dehydration8.
From a biochemical standpoint, the rhythm and depth of breathing directly influence carbon dioxide (CO₂) homeostasis and the body's acid-base balance. Excessive breathing causes CO₂ loss, shifts blood pH toward alkalosis, and promotes the excretion of minerals by the kidney, such as calcium, magnesium, and potassium12. In contrast, slower, controlled breathing elevates CO₂, lowers pH, and enhances oxygen release to tissues through the Bohr effect, thereby optimising cellular metabolism13.
In addition, haemoglobin's affinity for Oxygen depends on pH, CO₂, temperature, and 2,3- bisphosphoglycerate (2,3-BPG). In acidic environments such as metabolically active tissues, where CO₂ and lactic acid accumulate, haemoglobin releases Oxygen more readily. CO₂ facilitates this process by forming carbonic acid or binding to haemoglobin to form carbaminohemoglobin11. Meanwhile, 2,3-BPG, produced during glycolysis in red blood cells, further regulates oxygen delivery: elevated levels (as in hypoxia or high altitude) promote oxygen release. In contrast, reduced levels make haemoglobin retain Oxygen more tightly13. This entire mechanism is integrated with the bicarbonate-carbonic acid buffer system, maintained by the lungs and kidneys, which stabilises blood pH within the physiological range of 7.35–7.4512, 13.
The relationship between breathing and biochemical metabolism becomes especially evident during physical exercise. Increased glucose oxidation raises CO₂ production, intensifying acid-base adjustments and oxygen delivery. Nasal breathing during exertion enhances recovery, lowers heart rate, reduces lactic acid buildup by up to 40%, and improves endurance28. Additionally, the rise in muscle temperature facilitates Oxygen unloading, ensuring adequate supply to energy-demanding tissues. Chronic mouth breathing is associated with a range of structural and functional alterations that adversely affect respiratory efficiency and sleep physiology. These include craniofacial changes such as mandibular retraction, dental malocclusion (including overbite and crowding), airway and sinus obstruction, recurrent sinusitis, and headaches, all of which may compromise cerebral oxygenation. Studies show that up to 42% more water is lost during mouth breathing compared to nasal breathing. During sleep, particularly during REM phases, these alterations can disrupt sleep quality and interfere with endocrine regulation, notably by impairing vasopressin secretion 34.
From a therapeutic perspective, conscious breathing characterised by nasal inhalation, diaphragmatic activation, and a slow, regular, silent rhythm is fundamental for optimising respiratory function. Techniques such as Tough's orthophonic respiratory coordination and the 4-7-8 technique (inhaling for 4 seconds, holding for 7, and exhaling for 8 seconds) are proven effective in reducing chronic hyperventilation and improving overall well-being. However, this method can also be used temporarily to help individuals quickly recover their breath whenneeded[40]. Similarly, devices like Myobrace[41], designed to correct mandibular posture, show promise in restoring proper nasal breathing. In addition ,lung capacity naturally declines with age by approximately 12% in men and up to 30% in women, but targeted practices can counteract this trend [42,43]. Free diving, for instance, can increase lung capacity by up to 30%, while regular aerobic exercise improves it by around 15% [44].
Breathing less, through the nose and with prolonged exhalations, elevates PCO₂, enhances aerobic endurance, and boosts cardiorespiratory capacity (VO₂ max). The optimal breathing rhythm is considered to be about 5.5 breaths per minute, with inhalations and exhalations lasting roughly 5.5 seconds each37. Fundamentally, breathing acts as a true switch of the autonomic nervous system. Rapid, shallow breathing activates the sympathetic branch associated with stress and alertness, whereas prolonged exhalations reinforce parasympathetic dominance, fostering calm. This dynamic is tightly connected to metabolism: during aerobic activity, the ideal heart rate remains below the threshold calculated as 180 minus age (180-Age in years)43. Once surpassed, anaerobic metabolism predominates, with increased glucose consumption and lactate production. Accelerated breathing reduces PCO₂ (hypocapnia), shifts blood pH toward alkalosis, and promotes the loss of essential minerals and produces various symptoms, including fatigue, headaches, dizziness, sleep disturbances, and a sensation of breathlessness13, 30. Conversely, restrained breathing raises PCO₂, lowers pH, and facilitates oxygen release via the Bohr effect12. However severe acidosis may impair enzyme function, reduce oxygen delivery to tissues, and cause symptoms such as confusion, fatigue, and shortness of breath.
In addition, reduced CO₂ levels can also cause cerebral ischemia (diminished blood flow) and hypoxia (oxygen deficiency). Even a drop of just 1 mmHg in PCO₂ can decrease cerebral circulation by 2%, and a 22 mmHg in PCO₂, decrease can reduce it by up to 40%, leading to dizziness, tingling, confusion, psychosomatic sensations, or hypnagogic states, those transitional experiences between wakefulness and sleep. 29, 30. During breath holding, oxygen levels decline while CO₂ levels increase, leading to mild acidosis due to elevated blood CO₂ and a decreased pH. This reduction in haemoglobin's oxygen affinity enhances oxygen delivery to tissues, an expression of the Bohr effect11, 13.
To sum up, breathing less frequently, through the nose, and with prolonged exhalations enhances respiratory efficiency, maintains acid-base balance, optimises oxygen delivery, regulates the nervous system, and supports long-term health. In particular. For everyday life, a slightly slower and more balanced breathing pattern of around 4-5 breaths per minute is considered most appropriate, this respiratory rate optimises the synchronisation between breathing and heart rate, as been shown in addition to increasing heart rate variability, further promoting positive cardiovascular and nervous system balance. Taken together, these principles reveal that breathing is not merely an automatic mechanical act, but a powerful regulator of biochemistry, physiology, and mental state 23. The focus is on breathing holistically: light, slow, and deep.
Conclusions
In summary, the benefits of Pranayama encompass both physical and mental aspects, making it an essential practice for overall well-being.
Physical benefits: Regular practice improves lung capacity, strengthens the respiratory system, and regulates the nervous system, helping to balance bodily functions and promote better overall health.
Mental health benefits: Pranayama is an effective tool for reducing stress, enhancing concentration, and promoting mental clarity, providing a sense of calm and emotional stability.
Furthermore, breathing represents a unique physiological interface where multiple regulatory systems converge. It is simultaneously governed by autonomic control mechanisms and capable of voluntary modulation, creating a functional gateway between unconscious homeostatic processes and conscious behavioural influence. This bidirectional function positions it as a central regulatory axis through which individuals can exert measurable effects on autonomic activity, emotional regulation, and overall physiological equilibrium. The focus is on breathing holistically: light, slow, and deep, which influences the body's biochemistry and biomechanics and engages the autonomic nervous system. To sum up, "Breathe light to breathe right”.
Authors’ contributions
Both authors made valuable contributions to this manuscript. Each author drafted specific sections, and both actively participated in revising the entire document.
Declaration of AI Use
ChatGPT, an OpenAI language mode (version GPT-5.2, 2025),was used to support the writing process and improve clarity in certain article sections. It was not used to generate or alter the research results.
Abbreviations
References
- 1. (1997) Swami S.The Science of Pranayama. 16ª edición. The Divine Life Society, Shivanandanagar, Tehri-Garhwal, Uttar Pradesh, India. ISBN 81-7052.
- 2.Irzhak L I. (2005) . Christian Bohr (On the Occasion of the 150th Anniversary of His Birth).HumanPhysiology31(3) 366-368.
- 3.Çelik H, Yuruk E. (2025) The effect of the Buteyko breathing technique on asthma control and quality of life in children with asthma aged 7–12 years: A randomised controlled study.PeerJe19467.
- 4.Dienstmann G. (2018) Practical meditation. Penguin Random House, edited by Dorling Kindersley Limited, London WC2R ORL.
- 5.Olsson A. (2014) Conscious breathing. Amazon Italia Logistica S.r.l, Torrazza Piamonte(T) Italia. Third edition. , ISBN: 978-91.
- 6.Nestor J. (2020) Breath: The new science of a lost art. Riverhead Books. Penguin Random House LLC, ISBN 9780735213630.New , York .
- 7.McKeown P. (2015) The oxygen advantage. HarperCollins Publishers. , Great Britain, London, Piatkus, ISBN 978-349.
- 8.McKeown P. (2021) The breathing cure, OxyAt Books, ISBN: 978-1-909410-26-8. First edition. , Ireland
- 9.Telles S, Singh N. (2013) Science of the Mind: Ancient Yoga Texts and. Modern Studies. The Psychiatric Clinics of. , North America 36, 93-108.
- 10.Saraswati S S. (2002) . Asana Pranayama Mudra Bandha. 4th ed. Munger (Bihar): Yoga Publications Trust .
- 12.Berg J M, Tymoczko L, Gatto G J, Stryer L. (2023) . ed.). New York. NY: W. H. Freeman and , Biochemistry 10.
- 13.Hall John E, Michael Hall. (2020) . Guyton and Hall Textbook of Medical Physiology. 14ª ed. Philadelphia, PA: Elsevier Health Sciences. ISBN 978-0.
- 14.Anatomy Standring S Gray’s. (2020) . The Anatomical Basis of Clinical Practice, 42nd ed.2020 , Philadelphia, PA: .
- 15.Moore K L, Dalley A F, AMR Agur. (2023) Clinically Oriented Anatomy. 9th ed. , Philadelphia (PA):
- 16.Henderson Y, Haggard H, Scott S. (1922) The treatment of carbon monoxide asphyxia by means of oxygen+ CO2 inhalation: A method for rapid elimination of carbon monoxide from the blood.J. , Ame Ass 79, 1137-1145.
- 17.Paulus M P, Micallef J. (2013) Carbon dioxide inhalation as a human experimental model of panic: the relationship between emotions and cardiovascular physiology.Psychiatry Research209(1). 59-62.
- 18.Saper C B. (2002) The central autonomic nervous system: Conscious visceral perception and autonomic pattern generation.Ann Rev ofNeurosc25. 433-469.
- 19.Roderik J S, Band G. (2018) Breath of Life: The Respiratory Vagal Stimulation Model of Contemplative Activity.Frontiers in Human Neuroscience12:. 397-10.
- 20.Resenberg S. (2017) Accessing the healing power of the vagus nerve. North Atlantic book Barkely. , California
- 21.Shaffer F, Ginsberg J P. (2017) An Overview of Heart Rate Variability Metrics and Norms. Front. in Public Health 5 258-10.
- 22.Laborde S, Mosley E, Thayer J F. (2017) Heart Rate Variability and Cardiac Vagal Tone. in Psychophysiological Research – Recommendations for Experiment Planning, Data Analysis, and Data Reporting. Frontiers in Psychology 8 213-10.
- 23.Jerath R, Edry J W, Barnes V A, Jerath V. (2006) Physiology of long pranayamic breathing: neural respiratory elements may provide a mechanism that explains how slow deep breathing shifts the autonomic nervous system. 67(3), 571-10.
- 24.Eckberg D L, Sleight P. (1992) . Human Baroreflexes in Health and Disease , Oxford, UK, Clarendon .
- 25.Salah H M. (2024) Baroreflex function in cardiovascular disease: A review of mechanisms and therapeutic implications.Autonomic Neuroscience: Basic andClinical258. 102944-10.
- 26.Alvarez-Araos P, Jiménez S, Salazar-Ardiles C, Núñez-Espinosa C, Paez V. (2024) Baroreflex and chemoreflex interaction in high-altitude exposure: possible role on exercise performance. , Fro in Phy 15, 1422927-10.
- 27.Fincham G W. (2023) High ventilation breathwork practices: An overview of their physiological effects and safety considerations. , J of Psychoph and Clin Neurosci 45(4), 123-135.
- 28.Telles S, Naveen K V. (1997) Effect of alternate nostril breathing on autonomic functions in healthy young adults.Ind. , Jour of Physio 41(4), 467-472.
- 29.Kerr W, Paut A, Dalton J. (1938) Physical phenomena associated with anxiety states: the hyperventilation síndrome. California and western medicine 48;12.
- 30.Sigholm G, Ebert D, Hallström I. (1999) . Anxiety, pCO and cerebral blood flow.Psych Research88 3, 251-260.
- 31.Upadhyay J, Nandish N S, Shetty S, Saoji A, Yadav S S. (2023) Effects of Nadishodhana and Bhramari Pranayama on heart rate variability, auditory reaction time, and blood pressure: A randomised clinical trial in hypertensive patients. , J of Ayurv and Integra Medic 14(4), 100774-10.
- 32.Yadav A, Kaushik R M, Kaushik. (2021) Effects of diaphragmatic breathing and systematic relaxation on depression, anxiety, stress, and glycemic control in Type 2 diabetes mellitus. , Inte J of Yoga Therapy 31(1), 19-00061.
- 33.Wilson T, Baker S E, Freeman M R, Garbrecht M R, Ragsdale F R. (2013) Relaxation breathing improves human glycemic response. , The J of Alter and Compl Med 19(7), 633-636.
- 34.TorresCastro R, SolisNavarro L, Puppo H, AlcarazSerrano V, VasconcelloCastillo L. (2022) Respiratory Muscle Training. in Patients With Obstructive Sleep Apnoea: A Systematic Review and MetaAnalysis.Clocks & Sleep4(2): 219229-10.
- 35.Gautam S, Tolahunase M, Dada R. (2019) Impact of yoga-based mind-body intervention on systemic inflammatory markers and co-morbid depression in active rheumatoid arthritis patients: A randomised controlled trial. , Res Neu and 37(1), 41-59.
- 36.Callaham M.Hypoxic hazards: traditional paper bag rebreathing in hyperventilating patients. , Annals of Emerg Med 19, 145-149.
- 37.Lin I, Tai L, Fan S Y. (2014) Breathing at a rate of 5.5 breaths per minute with an equal inhalation-to-exhalation ratio increases heart rate variability.IntJ of Psy 91. 206-211.
- 38.Sing U P. (2017) Evidence-based role of hyperventilation and the exhalation phase in vagus nerve stimulation: insights into hypercapnic Yoga breathing exercises. , J Yoga Phys Ther 7, 276-2.
- 39.Schierbauer J, Zimmer R, Wachsmuth N, Maassen N, Schmidt W. (2024) . Plasma Volume Shifts and Acid–Base Balance After a Single Bout of Resistance Training.Journal of Science in Sport and Exercise124 4, 1061-1072.
- 40.Vierra J, Boonla O, Prasertsri P. (2022) Effects of sleep deprivation and 4-7-8 breathing control on heart rate variability, blood pressure, blood glucose, and endothelial function in healthy young adults.Phys Rep 10(13). 15389-10.
- 41.Luca L, Persano R, Piantanida S, Carganico A, Deppieri A. (2023) . The Effects of the Myobrace® System on Peripheral Blood Oxygen Saturation (SpO) in Patients with Mixed Dentition with Oral Dysfunction.Dentistry Journal11 8, 191-10.